A25-year-old woman with no relevant medical history developed fever, generalized body pain, dry cough, anosmia, and ageusia in April 2020. She was diagnosed with coronavirus disease 2019 (COVID-19) by positive findings on polymerase chain reaction assay and positive findings on computed tomography of the chest. Her clinical course was uncomplicated, and she was treated conservatively. Anosmia and ageusia started to improve during the following month. However, during the recovery phase, she started to experience offensive odor (cacosmia) and taste (cacogeusia) with stimulation of these sensations. Ear, nose, and throat evaluation showed normal clinical and endoscopic nasal examination findings. Computed tomography findings of the paranasal sinuses were unremarkable. She was given oral and intranasal corticosteroids, in addition to multivitamins, zinc, and olfactory training. However, her symptoms persisted for 3 months, and she was referred to our neurology clinic for further evaluation. Findings of her neurological examination were normal.
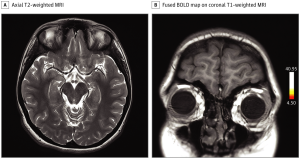
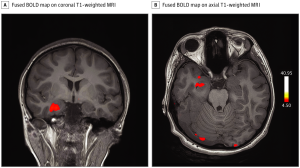
Magnetic resonance imaging (MRI) of the brain revealed normal findings, including the olfactory bulbs and sulci, which showed no structural or signal abnormality . A task-based functional MRI (fMRI) study was designed as alternating blocks of smell activation by a pleasant scent intervened with periods of rest. Blood oxygen level–dependent (BOLD) activation maps were generated and fused to T1-weighted multiplanar images. There was absent activation in the region of the orbitofrontal cortex (OFC), while the right uncus/piriform cortex demonstrated strong BOLD signal.
Link: https://jamanetwork.com/journals/jamaneurology/fullarticle/2775589